
In the United States, the joy of bringing new life into the world can be shadowed by a systemic failure of equity.
The sobering reality: a public health crisis that disproportionately claims the lives of Black mothers and their babies, a crisis that is acutely experienced in Allegheny County.
This is a systemic failure that spans from the federal level down to our own neighborhoods is not merely a matter of individual health choices.
We must first understand the depth of the crisis, its causes, and the movement currently working to dismantle the status quo, to begin working on solutions.
First, let’s understand the terms maternal mortality and infant mortality as defined by the CDC:
Maternal Mortality: the death of a woman while pregnant or within 42 days of termination of pregnancy, from any cause related to or aggravated by the pregnancy or its management, excluding accidental or incidental causes.
It specifically focuses on deaths resulting from pregnancy complications or chains of events initiated by pregnancy.
Infant Mortality: the death of a live-born baby before their first birthday (0–364 days)
The State of the Crisis: By the Numbers
National Overview
Nationally, Black women are three times more likely to die from pregnancy-related causes than White women, regardless of income or education level.
According to the CDC, the maternal mortality rate for Black women in 2023 was 49.4 deaths per 100,000 live births, compared to 14.5 for White women.
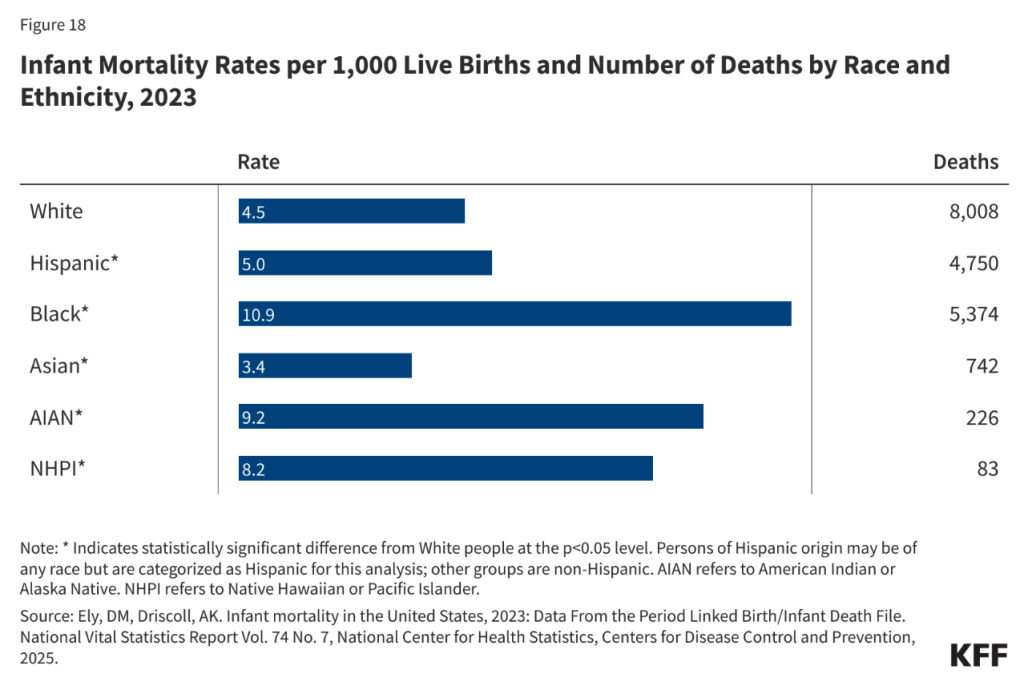
Similarly, the Black infant mortality rate remains more than double that of White infants. It is important to remember that this issue is not isolated to the Black community.

American Indian/Alaska Native (AIAN) and Native Hawaiian/Pacific Islander (NHPI) communities face the same crisis as their babies are dying at comparable rates
These national disparities in maternal and infant mortality rates are reflected in the data from Pennsylvania and dwarfed by the statistics in Allegheny County.
Pennsylvania (PA)
The disparity persists in the Commonwealth. According to the Pennsylvania Maternal Mortality Review Committee (MMRC), Black women account for a disproportionate share of pregnancy-related deaths. While they make up about 14% of births in PA, they represent nearly 30% of pregnancy-associated deaths.
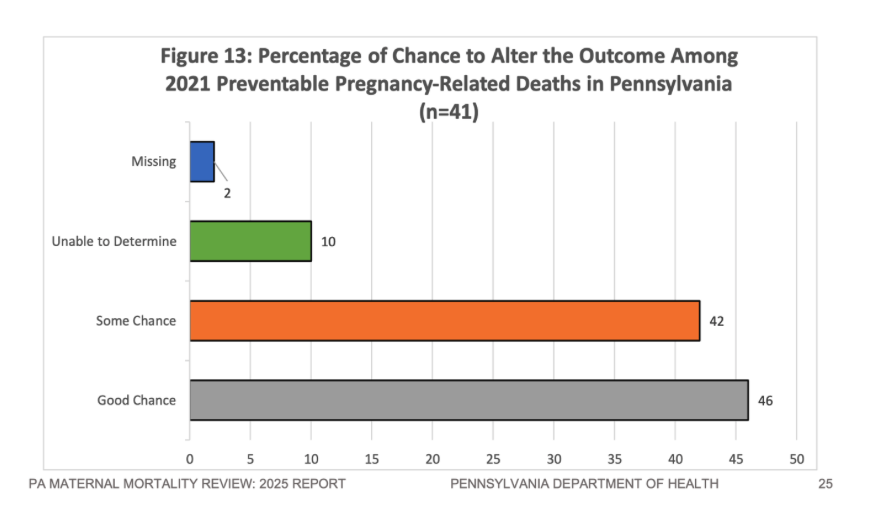
The MMRC found that up to 98% of these deaths are preventable. This means we aren’t fighting an incurable disease; we are fighting a fixable system.
Preventable death is defined by the MMRC as ‘at least some chance of the death being averted by one or more reasonable changes to the patient, family, provider, facility, system, and/or community factors.’
In addition to laying out the scope of the crisis the committee offered recommendations for improvement including:
· Improve access to high-quality care
· Addressing social determinants of health
· Improving rural health and maternity care deserts
· Supporting behavioral health and substance use disorder needs
· Expanding and diversifying the maternal health workforce
Allegheny County
Locally, the data presented in Pittsburgh’s Inequality Across Gender and Race report is even more jarring: Black women in Pittsburgh have higher maternal mortality rates than Black women in 97% of similar U.S. cities.
Discover the systemic causes, local data, and how the PA Momnibus 2.0 aims to achieve birth equity.
In addition, research from the Allegheny County Health Department and the University of Pittsburgh has shown that Allegheny County infant mortality disparities for Black babies are two times higher than White fetal mortality.
The crisis is not abstract or distant. Pittsburgh’s health equity statistics prove this is affecting your family, friends, and neighbors.
Why are Black Mortality Rates Higher in Allegheny County?
The significantly higher rates of mortality are driven by a complex intersection of factors:
- Systemic Racism and Implicit Bias: Healthcare providers may downplay the pain or concerns of Black patients, leading to delayed diagnoses of life-threatening conditions like preeclampsia or hemorrhage.
- Social Determinants of Health: Lack of access to stable housing, nutritious food, and reliable transportation in predominantly Black neighborhoods.
- The Coverage Gap: Inconsistent access to postpartum care after Medicaid benefits expire, though this is changing thanks to postpartum Medicaid extension in Pennsylvania.
How We Address the Causes of Black Maternal and Infant Mortality
This crisis requires more than just “better doctors”.
It requires a fundamental restructuring of how we treat Black mothers and their babies. We must move past simply acknowledging the problem and start implementing these proven, multi-layered solutions.
Here is an expanded look at how we address the root causes, along with the organizations and research driving these changes.
1. Eliminating Implicit Bias Through Standardized Care
Individual bias is a major driver of mortality and standardized clinical protocols (often called “Maternal Safety Bundles”) can override that bias by ensuring every patient receives the exact same life-saving interventions regardless of race.
2. Investing in “Culturally Congruent” Care
Research consistently shows that when Black mothers are cared for by Black providers (doctors, midwives, and doulas), they experience better outcomes, higher satisfaction, and lower levels of stress.
Doulas are a lifeline between the patient and a healthcare system that has historically been exclusionary. They are advocates, helping patients navigate the system and ensuring their pain and concerns are heard by medical staff.
Increasing the number of Black midwives and doulas and ensuring they are reimbursable via Medicaid is imperative.
3. Strengthening the “Fourth Trimester” (Postpartum Care)
Over 50% of maternal deaths occur after the mother has left the hospital, yet the standard of care has traditionally been a single check-up six weeks after birth. We can close the “coverage gap” where low-income mothers lose health insurance just as late-onset complications begin to surface.
Expanding Medicaid coverage from the standard 60 days to 12 months postpartum would ensure that mothers with preeclampsia, postpartum depression, or cardiac issues can continue to see doctors long after they’ve delivered.

4. Addressing Social Determinants of Health (SDoH)
Medical care accounts for only about 20% of health outcomes; the other 80% is determined by where someone lives, eats, and works.
Integrating Community Health Workers (CHWs) into prenatal care teams to help families secure stable housing, access nutritious food (WIC), and arrange reliable transportation to appointments is a good place to start.
Achieving health equity demands that we recognize the interconnectivity of healthcare with the other SDoH, and work to improve education, community, economic stability, and the built environment.
5. Centering Perinatal Mental Health
Black women are significantly less likely to be screened for or treated for postpartum depression and anxiety compared to White women, despite facing higher levels of stressors. Treating mental health as a vital sign of maternal wellness can prevent deaths.
According to the Policy Center for Maternal Mental Health, maternal mental health conditions (suicide and overdose) are the leading cause of maternal mortality, 20% of which are attributed to suicide.
The human toll is much worse in Pennsylvania. According to the 2025 Maternal Mortality Review Annual Report, mothers dying from MMH conditions is 47%, more than twice the national average.
The system must provide universal, culturally sensitive mental health screenings and support the creation of specialized support groups for Black mothers.
6. Diversifying the Medical Pipeline
We cannot fix the system without changing who is leading it. Currently, only about 5% of physicians in the U.S. are Black.
Supporting programs like the Black Maternal Health Momnibus, which provides scholarships and grants to increase the number of Black students in medical, nursing, and midwifery schools.
Fostering trust and improving communication begins with ensuring the workforce reflects the diversity of the patients they serve.
What is Being Done: Nationally, Regionally & Locally
National: The Black Maternal Health Momnibus Act
Led by the Black Maternal Health Caucus, the Momnibus Act is a transformative suite of 13 bills designed to:
- Invest in social determinants of health (housing, transport, nutrition).
- Provide funding for community-based organizations.
- Grow and diversify the perinatal workforce.
- Improve maternal health care for incarcerated moms and veterans.
- Invest in digital health tools and maternal vaccination.
Pennsylvania: The 2025 Strategic Action Report & Legislation
Pennsylvania is taking aggressive steps to rectify these disparities:
- 2025 Maternal Health Strategic Action Report: A.K.A ‘Healthy Moms, Vibrant Futures Action Plan’ outlines a roadmap for PA to improve outcomes by focusing on health equity, data transparency, and increasing the number of Black maternal health providers.
This MHSAR also includes investment to support perinatal programs, diversifying the workforce, and expand doula access.
- Legislative Action: The Black Maternal Health Momnibus 2.0 PA legislative pakcage includes bills to mandate implicit bias training for healthcare professionals and to provide Medicaid reimbursement for doula services, ensuring professional support is accessible to low-income families.
Local: Allegheny County Efforts
In Allegheny County, the Hello Baby program and the Birth Circle initiative focus on connecting high-risk families with resources.
Organizations like Healthy Start Pittsburgh provide direct home visiting services, while the Pittsburgh Black Breastfeeding Circle offers specialized peer support to improve infant health outcomes.
Get Involved: Take Action Today
We cannot wait for the statistics to change on their own. You can make a difference:
- Advocate: Contact your state representative to support the PA Momnibus bills.
- Donate: Support local doula funds that provide free services to Black birthing people.
- Educate: Share this blog and the resources below to raise awareness.
Maternal & Infant Community Health Resources (Pittsburgh & Allegheny County)
Comprehensive Maternal & Child Health Services
These organizations offer “one-stop” support, including prenatal care, home visiting, and health navigation.
- Healthy Start Pittsburgh: A cornerstone for Black maternal health in the region. They provide home visiting, doula services, fatherhood programs, and care coordination to improve birth outcomes.
- Allegheny County Health Department (Women, Infants & Children): The Women, Infants, and Children (WIC) program offers a variety of health and nutrition services for medically or nutritionally at-risk mothers and children
- The Midwife Center for Birth & Women’s Health: Located in the Strip District, they offer a personalized, wellness-based approach to birthing, including prenatal, postpartum, and gynecological care.
Doula & Birthing Support
Doulas provide physical, emotional, and informational support during pregnancy and labor.
· Birth Circle Doulas – UPMC Magee-Womens Virtual Care Center: The Birth Circle Doulas clinic offers consultative video visits with a specially trained labor and support person who provides non-medical comfort in every stage of pregnancy.
- Hello Baby: An Allegheny County initiative that offers three tiers of support. Depending on your needs, they can connect you with a “Family Support Center” or intensive home-visiting services that often include doula care.
- Pittsburgh Doula Network: Pittsburgh Doula Network has a network of trained and experienced doulas knowledgeable in newborn care, postpartum recovery, breast, chest, and bottle feeding, family support, and most importantly – care for the birthing person.
Breastfeeding & Lactation Support
Specialized support for nursing mothers to ensure a healthy start for infants.
- Pittsburgh Black Breastfeeding Circle (PBBC): A community-led group providing peer support and education specifically tailored to the experiences of Black families in Pittsburgh.
- The Breastfeeding Center of Pittsburgh: Offers professional lactation consultations, classes (online and in-person), and a boutique for nursing supplies.
- Allegheny County WIC (Women, Infants, and Children): Beyond food assistance, WIC provides breastfeeding peer counselors and lactation specialists at no cost.
Diapers, Clothing & Essential Supplies
If you are in need of diapers, wipes, or baby gear, these organizations bridge the gap.
- Western Pennsylvania Diaper Bank: Works through partner agencies across the county to provide diapers and period products to families in need.
- Genesis of Pittsburgh: Provides a “Learning Center” where mothers can earn “boutique points” for baby clothes, diapers, and gear by attending classes. They also offer free pregnancy testing and counseling.
- Beverly’s Birthdays (Baby Showers): Hosts “community baby showers” for expectant parents and provides “newborn care packages” to families in need.
Food & Nutrition Services
Ensuring you have access to nutritious food is vital for a healthy pregnancy.
- Greater Pittsburgh Community Food Bank: Offers several programs, including “The Doorstep” delivery and drive-up distributions across Allegheny County.
- 412 Food Rescue: Uses an app-based system to redistribute fresh food to community centers and housing complexes.
- Adagio Health: Provides WIC services and nutritional counseling at multiple locations throughout the county.
Emotional & Mental Health Support
Perinatal mental health is a vital sign of overall wellness.
- The Maya Organization: Provides specialized counseling for expectant and new mothers, along with prenatal classes and parenting support groups.
- Postpartum Support International (PA Chapter): Connects mothers with local therapists who specialize in perinatal mood disorders and offers free online support groups.
- Neighborhood Resilience Project: Located in the Hill District, they offer trauma-informed community support and health navigation for families.
Not sure where to start?
Dial 2-1-1 or visit PA 211 Southwest. They can provide immediate referrals for housing, utility assistance, and emergency food services based on your specific zip code.
Additional Resources
National Resources
- Legislative: Black Maternal Health Caucus – According to the BMHC, the caucus has enacted over $200 million in new Momnibus and maternal health funding through the federal appropriation process since 2023.
Curious where the money is going? You can track the dollars here.
- Research: Black Mamas Matter Alliance (BMMA) – Leading research and advocacy on Black maternal health.
- Educational: CDC Hear Her Campaign – Education on maternal warning signs.
Regional Resources (Pennsylvania)
- Legislative: PA Black Maternal Health Caucus – Keep up to date on state-level policy information.
- Research: Pennsylvania Perinatal Quality Collaborative (PA PQC) – Improving clinical outcomes across PA hospitals.
- Educational: PA Department of Health Maternal Health Page – State-specific data and reports.
Local Resources (Allegheny County)
- Legislative: Allegheny County Council – Engage with local policymakers on health funding.
- Research: The Center on Social Disparities in Health (Pitt) – Localized research on health gaps.



